Ben’s Story in Periodontics
Last time I said I would tell you my story, but before I do, perhaps it would be helpful to define in general terms, what success in periodontal therapy ought to look like.
When Periodontal Therapy is running smoothly in the dental office:
- Most periodontal disease is being detected early.
- Most patients diagnosed with periodontal disease are accepting care.
- Most patients assume personal responsibility for effective daily plaque control and the management of reasonable appointment intervals.
- Patients and the office team work well together and morale in the office is high.
- Therapy follows predictable and positive paths toward good dental health which is reflected in easy to understand documentation.
- Referrals grow through word of mouth in part due to the success of the periodontal therapy program in the office.
- When therapy is not working, patients don’t blame and dentists don’t hide. Consultations and collaboration with others help move patients toward more sophisticated therapeutic options. In other words, no one is falling into supervised neglect.
Last time I ended with:
“Fundamentally, successful periodontal therapy is rooted in persuasion. Yes, technical skills are important, but long-term there is more required than this. I believe much of it is about engaging people in a story that gives them the road-map they can follow to better dental health. I call this the dentist’s story.
To help explain this, let me demonstrate it by telling you a little bit about my story in dentistry, especially as it relates to periodontal therapy. This, I think, will also help explain why general dentists have less interest in periodontal disease than do dental hygienists and periodontists.”
So here it is:
Ben’s Story in Periodontics
Dental School Lectures:
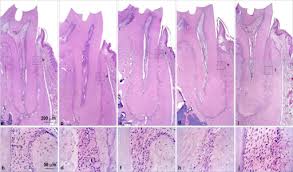
My recollection of the first lectures in periodontics seemed to involve histology slides. Usually they were of the cross-section of teeth with alveolar bone and soft tissue showing inflammation and the loss of attachment. I recall that the instructor had a lot to say, but the slides didn’t seem to change very much, if at all, lecture after lecture…
Honestly, what I really wanted to know was what would be on the test. I relate to the statement that dental students really have only two goals in life. The first is to get into dental school, and the second is to get out.
Dental School Clinic:
I remember spending hours probing and recording pocket depths. I also remember scaling and root planing and hoping that my work would be adequate to enable me to do more interesting things, like crown and bridge. One time following a quadrant of scaling and root planing I noticed that I had received a reduction in my grade, so I asked the instructor what I had done wrong. He said I injured some soft tissue. Had I not asked, he would not have told me this much. Having asked, I didn’t really know what I should have done differently. The whole thing seemed subjective and mysterious.
As dental students, when my classmates and I couldn’t get our patients past the periodontics department in order to move them forward to other care, we called this the “Perio Penalty Box.”
I assisted a perio resident in one surgery on one of my patients as per graduation requirements. I remember he reflected a flap and I got to see a bony defect. Beyond this I have no idea what he did.
Only the nerdiest among us considered specializing in periodontics upon graduation from dental school.
Air Force General Practice Residency:
So I finished dental school with no particular fondness for periodontics, and because the Air Force paid my way through it, upon graduation, I went on active duty in order to payback the incurred obligation. In my first year, the Air Force wanted to take me back through every clinical dental discipline one more time. Since I was now happily earning a living for the first time, this was just fine with me, although, I have to be honest and say, I didn’t think they could really teach me very much more than I had already learned. This turned out to be one of the dumbest beliefs I have ever had. In one year in this residency my knowledge and skills at least doubled over the previous four.
As for periodontics, it was in this residency that I began to really understand this fascinating and important field for the first time. This is because I was now following the response to treatment over longer time intervals and it wasn’t connected with my fixation on graduation. In the residency, personal performance pressures came off and I could simply observe how tissues and people responded to treatment. For example, I started to better appreciate what the patient could do personally to improve gingival health through better daily home care practices. I also began to see what happens following scaling and root planing and a variety of surgical procedures I actually was taught to perform.
Sometimes results were remarkably good and other times not so good. I began to appreciate what I could and couldn’t do for people and to what extent their cooperation in the process was fundamental. I would have been happy to cure people if that was a possibility, but it really wasn’t. And since it wasn’t, then I needed to know what I could do to help and where some patients’ expectations may not be in line with reality.
Let me also add that this residency within the military afforded me an opportunity many other dentists never receive and that is this. While I was developing my clinical skills, the financial elements found in private practice did not affect me or my patients. This allowed me to simply concentrate on therapeutics unclouded by worries about what patients could and could not afford.
Hahn Air Base:
But my story didn’t stop there. In my first real assignment I was one of about eight general dentists at a midsized dental clinic in Germany. The only specialist in the bunch was a prosthodontist.
A fellow resident from Barksdale and I reported for duty together. The clinic was in the midst of an expansion that would double its size. This meant that the single hallway off of which every dental treatment room was connected would grow to be over half a football field in length. Our new boss, a dentist with the rank of colonel, told us he wanted one of us to concentrate doing root canals and the other to focus on periodontics.
Then we were shown our assigned rooms.
My friend’s operatory was directly across the hall from the single X-ray machine in the building. I had the room furthest from X-ray. That’s when I volunteered to do perio. It is not really an exaggeration to say I ultimately became a periodontist because of a long hallway. Perhaps I’m hoping it’s not because I’m nerdy.
At this clinic I was now seeing a large population of periodontal patients. Each one needed similar upfront information and treatment. I found my explanation about what periodontal disease is and how it is treated after being repeated hundreds of times developed into a very smooth, logical and standardized presentation. I could give it in my sleep and every word was justified or eliminated. Interestingly I think I started in a way similar to my first dental school professor with the cross section of that tooth. More about this later.
Periodontics Residency:
Three years. Very hard. I survived.
Obviously I now understand the discipline of periodontics at a deeper level, but the patient-flow elements did not dramatically change because of this residency.
Instructor in an Air Force Advanced Education in General Dentistry Program:
This was similar to my GPR. They had simply changed the name. I had come full circle in my Air Force career. Now I was the periodontist working with recent dental school graduates. This lasted five years and then on to my last military assignment.
Director of the USAF Periodontal Therapist Program:
We trained enlisted personnel to function as dental hygienists. Eventually after I retired they created the educational bridges to enable these individuals to challenge state examinations and become civilian dental hygienists upon retirement. As the head of this program I had the opportunity to further refine and standardize the patient education piece that I will share with you in the coming posts.
Conclusion:
I have worked with thousands of patients and have been involved with the training of hundreds of dentists, dental hygienists or their equivalent. This has resulted in the development and refinement of a process of patient instruction and therapeutic interaction that is easy to understand, train and implement. It addresses the treatment and management of chronic periodontitis in a way that enables patients to get better and dentists and their teams to not assume responsibility for parts of therapy they cannot directly control. In addition it helps general dentists and periodontists work cooperatively when necessary on behalf of those patients with more advanced problems.
I have learned over the years that periodontal therapy has the best chance of long-term success when patients are instructed and given personal responsibility as early as possible. If you decide to follow my advise, this may change how patients are informed and taught at the beginning of care in your clinic. A little more time may need to be invested in informing and training the patient, however the payoff will come when therapy moves smoothly and when patients understand without difficulty when eventually additional therapeutic measures become necessary to recover or sustain periodontal health.
And as an additional bonus, I have discovered it is easier working with the office team when everyone knows the dentist’s story and can explain it to patients. When this happens patients are reinforced by different individuals over time who simply review the relevant statements the patient has been hearing from the very beginning. We might call this the echo effect.
On the other hand, I have also seen poor results when dentists have pressed into treatment too quickly before the patient was adequately briefed on his or her important role in therapy. When this happens patients automatically assume that everything will be just fine because of what the dentist or dental hygienist does. In other words, a less than stellar outcome has nothing to do with what they personally do or fail to do. And when they are never told differently, their conclusion is understandable. Unfortunately later, when results do not last and these patients see other dentists, they may be told that the treatment provided earlier was substandard. At this point everyone will be looking back at the documentation. What was the patient told? Can you prove it? When the office follows a general scripted plan such as the one I will share shortly, the answer will be most certainly Yes.
Next Time: The Power of Stories.
__________________________________________________________________________________________________________________
What you are reading is a section out of a manuscript I am writing on Periodontal Therapy. If this topic interests you, and you want to make sure you get the whole document once it is completed, please send me an e-mail with your request and I will add your e-mail address to the list. This list is confidential and will not be sold or given away.
Also understand that I am deputizing you to be part of my editorial team. Your comments, corrections, and even encouraging words are definitely appreciated. Also you have my permission to forward my writing to others you believe might be interested.
Finally, should you be interested in me providing this information live, pass a recommendation on to dental meeting planners. If you are a periodontist and would like me to train you, your team, along with your referring dentists and their teams, in a more personal and hands-on manner, please drop me a line.